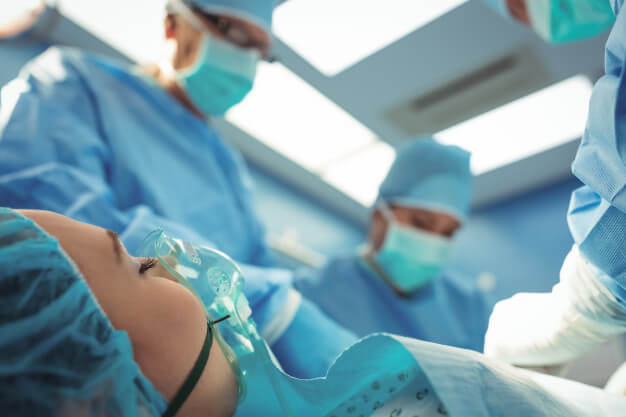
Anesthesia is a medical treatment that prevents the patient from feeling pain during the surgery. The medication is safe and is infused intravenously in the body before surgery. A specialist known as Anesthesiologist gives you anesthesia and takes care of you before, during, and after surgery.
To brief the mechanism of anesthesia, anesthesia works by interrupting the nerve signals in the brain and body. Various medicines that are infused intravenously help induce sleep.
Today, anesthesia works to achieve four goals, to make sure that you have no pain, that you’re asleep or unconscious, that your body doesn’t move so that the surgery can be performed on it, and that you aren’t left with any sign of an unpleasant memory of the procedure. Read on to know about the various types of Anesthesia, its uses, symptoms, and complications.
1. What are the Types of Anesthesia?
Local anesthesia
Unless you’ve made it through life without extracting your wisdom teeth or had an injury needing stitches, you’ve definitely had local anesthesia. Local anesthetic medicines are administered near the area to be treated, and their results are limited to only a small area.
Typically, they are provided by a professional nurse, dentist, or doctor who must ensure the region is numb. In reality, giving local anesthesia does not necessitate specialized training. Although you may not feel pain with local anesthesia, you may feel some symptoms of pressure. If that causes discomfort, ask your Anaesthetic Doctor for a sedative to ease your worry.
Regional anesthesia
Local anesthetics are administered via regional anesthesia near nerve clusters to numb a wider area, or region, of the body to manage pain. A common example is hand surgery where, depending on the type of numbing medication used, a shot of numbing medication near the nerves in the armpit can help make the whole arm go numb for three to 24 hours.
Neuraxial anesthesia
Neuraxial anesthesia involves spinal and epidural anesthetics. Numbing medication is positioned near the spinal roots in neuraxial anesthesia, leaving an even greater portion of the body numb than regional anesthesia does.
Epidurals are generally prescribed to manage labor and childbirth pain, or pain caused by a broad incision of the abdomen. Spinal that block the abdominal and lower body sensations are frequently used for cesarean sections and knee surgeries.
Limited Sedation
It’s surprising to note that with regional and neuraxial anesthesia, you will be able to choose how conscious you are during the operation. You’ll be comfortable with limited sedation but you will be mindful of what’s going on.
Moderate sedation will put you under a “twilight sleep,” in which you drift into and out of consciousness but can easily be aroused. You are practically fast asleep with deep sedation and are unable to recall anything.
General Anesthesia
General anesthesia affects the whole body and leaves patients unconscious and unable to move. They may have difficulty remembering things once it wears off. This is used by surgeons when operating on internal organs and for other invasive or time-consuming procedures like back surgery.
Many major, life-saving operations will not be feasible without general anesthesia. This includes open-heart surgery, brain surgery, and organ transplants.
Administration
Physicians administer general anesthetic either directly (intravenously) into the bloodstream, or as a gas which is inhaled by the patient. General intravenously injected anesthesia works rapidly and easily vanishes from the body. It helps patients to return home faster following surgery. Anesthetics inhaled can take longer to wear off.
Possible Side Effects
General anesthesia is usually safe. Age is an important factor for possible side effects. But for certain patients, such as the elderly or people with chronic illnesses like diabetes, they can pose risks. In certain patients, mostly children, side effects can also persist for many days and must be monitored carefully everyday.
Though there are some risks, as with any medical procedure. Specialized doctors called anesthesiologists closely monitor unconscious patients to reduce these medical complications, and may change the amount of anesthetic they get. Patients may sometimes need additional therapy for health management.
2. How to Plan your Anesthesia Procedure?
When you are having a procedure requiring regional, neuraxial, or general anesthesia, you may have a pre-operative consultation with an anesthesiologist, nurse, or physician assistant a few days before your operation.
It ‘s important to let the doctor know all the medications you’re taking every day. You will also be asked whether you have ever had an adverse reaction to anesthesia and whether you have ever been reliant on drugs, alcohol, or other substances.
The knowledge will help you determine the type of anesthesia you are getting. You should be able to select between regional, neuraxial, and general anesthesia for several procedures depending on your age.
In certain cases, a combination may be a better option. For example, even if general anesthesia is required, a regional block or epidural can also be provided to help with pain management after surgery, minimizing the need for narcotic pain relievers when you recover.
Using regional or neuraxial anesthesia often decreases the amount of general anesthesia you need, and thus side effects such as delirium, nausea, and delayed bowel and bladder function are less likely to manifest.
3. What does a Physician Anesthesiologist do?
According to Mayo Clinic, your anesthesia team is responsible for overseeing all changes in your health condition and wellness including heart rate, blood pressure, and, in general, blood and oxygen delivery to your organs while at the same time keeping you unconscious and relaxed during your operation, so that you are pain-free and comfortable. Gradually the anesthetic will wear off and you’ll wake up in the intensive care unit with improved health.
4. Will my mind work the same after being administered anesthesia?
Postoperative cognitive dysfunction (POCD) is the term used to describe a potential loss in memory, quick reasoning, or behavioral changes that may be the outcome of a general anesthesia cardiac operation.
Anesthesia Awareness Facts reveal that many patients can experience this health condition after surgery for a few days or weeks, but most are back to normal health within two to three months.
Doctors from Cleveland recommend staying as healthy as possible before surgery, and get active quickly after the procedure to reduce the risk of infections and other overall complications to improve recovery speed.
5. Will I wake up in pain afterward?
The comfort, wellness, and health of patients are top priorities for physician anesthesiologists. Some of the heavy pain medications slow your breathing, so they will balance medications to keep you relaxed while monitoring your respiratory functions. Physician anesthesiologists operate to relieve pain using a wide variety of medications, and they’ll try to alleviate the discomfort if you don’t feel relaxed when you recover from anesthesia.
Conclusion
Today, most anesthesia wears off pretty fast, however, following surgery you can still feel groggy, have a loss of memory, or have poor judgment and have no idea what’s going on. For the first 24 hours after surgery, people are advised not to make any big life decisions or drive a car or run machinery. You may also be advised for extra therapy. We suggest that you consult with your healthcare clinic’s anesthesia team openly about any questions or concerns you may have before the surgery.